
With the rapid development of diagnostic techniques and the widespread use of screening tests, an increasing number of patients with cervical cancer are diagnosed at an early stage. It was estimated that 569,847 new cases of cervical cancer were diagnosed and that 311,365 women died of this disease globally in 2018 1. The patients with common iliac LNM had poorer survival than those with LNM confined to the lower pelvis, while the differences in survival between patients with LNM confined to one node, one region or single side and those with more widely spreading LNM were not statistically significant.Ĭonclusions: Tumour size, LVSI and age are region-specific risk factors for pelvic LNM in IB1 cervical cancer, which could be used to allocate the appropriate extent of pelvic lymphadenectomy.Ĭervical cancer is one of the most frequent malignancies in women. A nomogram of these two factors showed good calibration and discrimination (concordance index, 0.761 in the primary cohort and 0.830 in validation cohort). The negative predictive values of tumour size 50 years) for obturator LNM were 100% and 98.7%, respectively. Among others, tumour size and lymph-vascular space invasion (LVSI), which are preoperatively assessable, were identified as independent risk factors of LNM in the common iliac region and the lower pelvis, respectively, and age was an additional independent risk factor of obturator LNM. The incidences of LNM at the obturator, internal iliac, external iliac, common iliac, and parametrial regions were 8.5%, 5.4%, 4.7%, 1.9% and 1.8%, respectively. Results: LNM was found in 266 (1.3%) removed nodes and 106 (14.6%) patients. Overall survival and progression-free survival in patients with different LNM patterns were compared. The performance of the nomogram was assessed by its calibration and discrimination. Nomograms were generated from the primary cohort and validated in another external cohort (N=242). The risk factors for LNM in different anatomic regions (obturator, internal iliac, external iliac, and common iliac) were evaluated by multivariate logistic regression analyses. All removed pelvic nodes ( N=20,134) were pathologically examined. Methods: A primary cohort of 728 patients with stage IB1 cervical cancer who underwent radical hysterectomy and systematic pelvic lymphadenectomy were retrospectively studied. 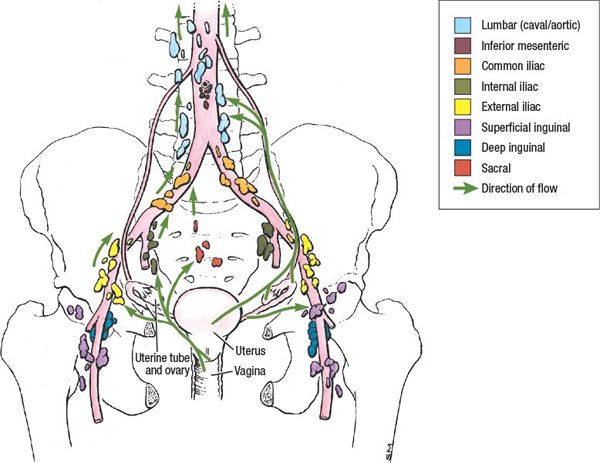 
Objectives: We aimed to identify the risk factors associated with pelvic lymph node metastasis (LNM) at each anatomic location in patients with stage IB1 cervical cancer.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
